Renin / Angiotensin / Aldosterone / ANP
Aldosterone:
. Mineralocorticoid hormones such as Aldosterone act in the kidney to stimulate active Na+ transport by the distal convoluted tubules -----> net result Na+ retention.
. These hormones promote the secretion of K+, H+ and NH4+ by the kidney and affect ion transport in other epithelial tissues including sweat glands, intestinal mucosa, salivary glands.
. As a result of shifts in electrolyte distribution there are changes in volume of fluid compartments within the body.
. Large doses of mineralocorticoids increase both extracellular fluid and circulating blood volume.
. Aldosterone is the most potent naturally occurring mineralocorticoid and accounts for most of the above actions in humans.
. Aldosterone is 25 times more potent than 11-deoxycorticosterone (DOC) and 1000 times more potent than cortisol or corticosterone.
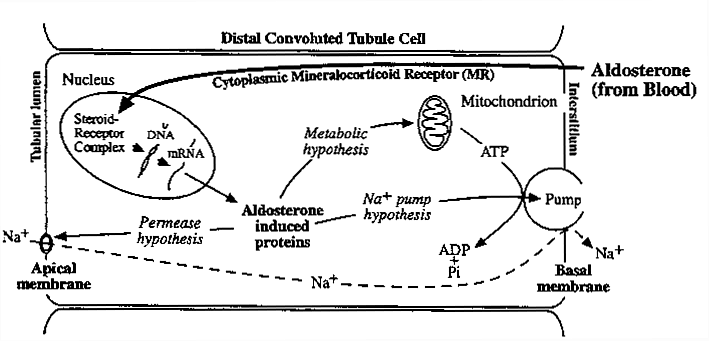
Mechanism of Action of Aldosterone:
Aldosterone works through a nuclear receptor to induce the formation of one or more proteins which in turn:
Increase the permeability of the membrane to Na+
Increase the active transport of Na+ out of the cell
Increase the energy available to the pump

i) The hormone-receptor complex binds to DNA and alters the rate of transcription of specific genes.
ii) Na+ enters passively through Na+ channels.
iii) Na+ is then transported by the Na+/K+ dependent ATPase pump. (ATP as energy source)
iv) Aldosterone increases the number of membrane Na+ channels.
v) Aldosterone increases the activity of several mitochondrial enzymes (i.e. citrate synthase). Most likely resulting in the generation of ATP to drive the ATPase pump.
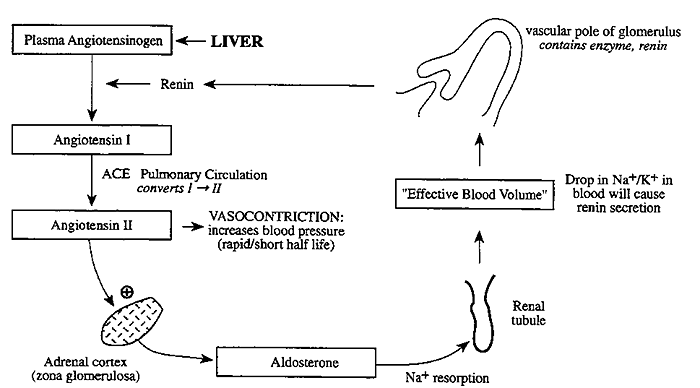
Renin-Angiotensin System:
- The system involved in the regulation of blood pressure and electrolyte metabolism.
Formation and Metabolism of Angiotensin II:
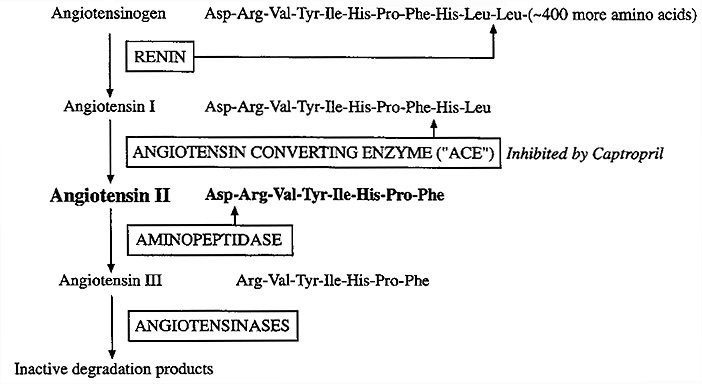
i) Angiotensinogen, synthesized in liver (+ glucocorticoids and estrogens), is the substrate for renin, an arterial enzyme.
ii) Renin acts upon angiotensinogen to produce angiotensin I.
iii) Hypertension associated with these hormones may be due in part to increased levels of angiotensinogen. Since it circulates at about the same Km (binding affinity) for renin, small changes would markedly affect the generation of angiotensin I.
iv) Angiotensin-Converting Enzyme (ACE), a glycoprotein found in lung, endothelial cells and plasma, removes 2 carboxy-terminal amino acids from angiotensin I to form angiotensin II.
v) Various antagonistic peptide analogues of angiotensin II and drugs like Captopril (a suicide substrate that inhibits ACE) are used to treat renin-dependent hypertension.
Angiotensin II increases blood pressure by causing vasoconstriction of the arterioles and is the most potent vasoactive substance known.
Angiotensin II inhibits renin release in a short feedback loop and is a potent stimulator of aldosterone production. Aldosterone increases Na+ and H2O retention
Any combination of factors that decreases fluid volume (dehydration, decreased blood pressure, fluid or blood loss) or decreases in NaCl concentration (low Na+ intake) stimulates renin release.
This system is so sensitive that even a change from lying down to sitting up will increase renin secretion and lead to Na+ and H2O retention via aldosterone.
The Dynamic Control of the Renin-Angiotensin-Aldosterone System:
Atrial Natiuretic Peptide (ANP):
- The control of body sodium, water and blood pressure involves a complex interaction of hormonal and neural mechanisms.
- The major determinants include: central and autonomic nervous function, cardiac output, blood vessel tone, renal function, the renin-angiotensin-aldosterone system, catecholamines and antidiuretic hormone.
- It was recently found that the heart atrial muscle produces a polypeptide hormone, ANP, that interacts with several of the above determinants allowing for both long- and short-term regulation of salt and water balance, as well as blood pressure.
- Properties of ANP include: potent diuretic and hypotensive actions and an inhibitory effect on renin and aldosterone excretion.
Physiology and Biochemical Actions of ANP:
"ANP links the heart, kidneys, adrenals and the blood vessels"
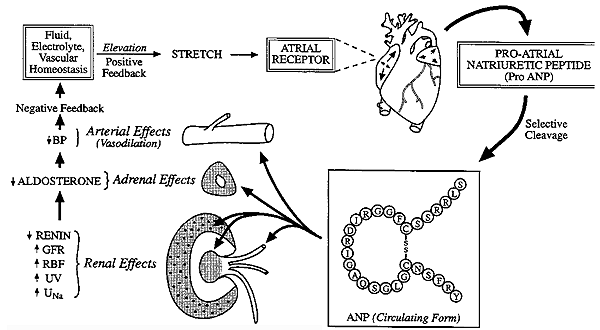
i) The ANP gene codes for a prepro-hormone.
ii) Loss of the hydrophobic leader sequence generates the 126 A.A. pro-hormone. Stored in granules of atrial myocytes.
iii) Increases in plasma levels of ANP can be elicited by atrial stretch caused by volume expansion, constrictor agents that elevate atrial pressure, immersion in water, atrial tachycardia, and high salt diet.
iv) The plasma active hormone is a low molecular weight carboxy-terminal fragment of 28 A.A.'s (ANP). A very selective enzyme cleavage of the pro-hormone occurs during the release process.
v) Once in circulation the peptide exerts a number of effects through specific cellular receptors to produce a multiplicity of actions involved in renal and cardiovascular functions.
Renal Effects of ANP:
Decreases Renin Secretion
Increases Glomerular Filtration Rate (GFR)
Increases Renal Blood Flow (RBF)
Increases Urine Volume (UV)
Increases Sodium Excretion (UNa)
Adrenal Effect of ANP:
Decreases Aldosterone Secretion
Atrial Effect of ANP:
Vasodilation Leading to a Decrease in Blood Pressure
Hypothesized Antagonistic Relationship Between ANP and the Renin-Angiotensin System in the CNS and Periphery:
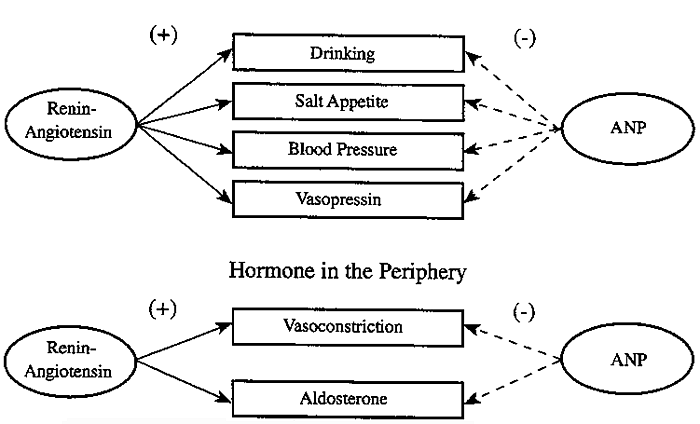
Receptor Mediated Mechanism of Action of ANP and Angiotensin II:
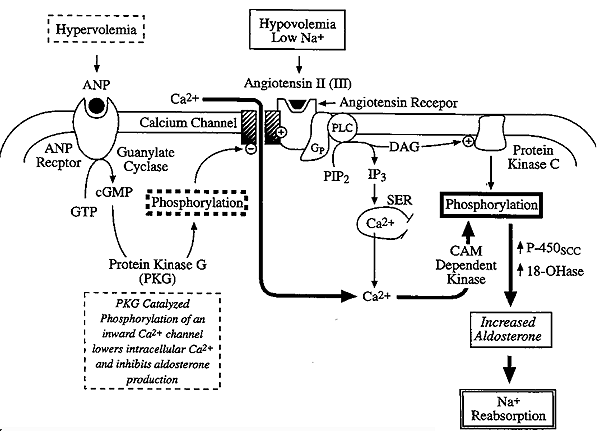
Angiotensin II binds to its receptor, which is coupled to a calcium channel and Phospholipase C via Gp to produce IP3/DAG.
IP3 enhances Ca2+ mobilization and CAM-dependent kinase plus PKC lead to phosphorylation of specific proteins.
These events activate P-450scc and 18-OHase to metabolize cholesterol to aldosterone.
Aldosterone produces increased Na+ Reabsorption.
ANP binds to its recepteor, which is coupled to the same calcium channel, producing cGMP from GTP and activating a novel serine/threonine kinase, Protein Kinase G (PKG).
PKG phosphorylates the calcium membrane channels to lower intracellular calcium levels thus decreasing Aldosterone levels.
© Dr. Noel Sturm 2015